No doubt our regular readers and listeners will have noticed that muscle is having a moment in the healthy aging conversation. In this article, I want to tease out the potential contribution of some additional interventions that we can think about clinically to support muscle health – the amino acid leucine, its derivative HMB (beta-hydroxy-beta-methylbutyrate), vitamin D and urolithin A. ~ DrKF
Why Muscle Health Is Critical for Healthy Aging
Skeletal muscle is not just for movement and balance, even as these are critical functions for healthy aging. It is also an endocrine organ in its own right, affecting our metabolism, inflammatory profile, and even brain function. Recent research shows muscle releases BDNF (brain-derived neurotrophic factor) that has effects both locally in neuromuscular junctions, helping maintain muscle quality, as well as in the brain where it promotes healthy cognitive function. Exercise increases muscle-derived BDNF and those increases are maintained in circulation for up to 24 hours post-exercise. Other myokines promote BDNF production in the brain. Low levels of BDNF impair neurotransmitter release and are associated with neurodegenerative diseases such as Alzheimer’s disease.
Muscle Loss – Strength vs Volume
Age-related muscle loss (sarcopenia, in its more extreme form) is what we tend to think of as the most universal muscle concern as we grow older. On average, we lose about 3-5% of our muscle volume per decade starting after age 30. However, another important but underappreciated consideration is what has been termed “dynapenia,” which focuses on the loss of muscle quality – function and strength – which also involves muscle neurological factors as well as muscle tissue itself. It’s important that we pay attention to both of these aspects.
When we’re younger, combining exercise with protein consumption pretty readily leads to building muscle. However, as we age, our bodies are less sensitive to the muscle-building effects of dietary amino acids – in other words, over time we develop muscle anabolic resistance. There are a few interventions we can think about to counter this, even as we continue with that all-important resistance training.
How Leucine Supports Muscle Protein Synthesis in Aging Adults
Leucine is an essential amino acid that activates mTOR (mechanistic target of rapamycin) signaling in skeletal muscle. What that does is to stimulate protein synthesis from amino acids. It also has other functions related to cell growth and metabolism. Incidentally, as the name suggests, it is also the target of rapamycin, which is considered a promising anti-aging agent. Studies of rapamycin in mice have shown increased lifespan, delayed age-related disease, and potential age reversal, although human effects have not yet been fully teased out.
We know from acute intervention studies, consuming about 3-4g leucine is necessary to activate the mTOR pathway and maximize muscle protein synthesis in older adults. This corresponds to about 25-30 g protein per meal. Unfortunately, older adults typically only achieve this level of protein intake at one meal per day. Other meals fall short on protein and leucine intake.
Another option may be to add leucine by itself. Studies investigating the addition of leucine supplementation to relatively low-protein meals have found that 4-5 g leucine with a regular meal can enhance protein muscle synthesis. When combined with a modest resistance exercise routine, this led to increased protein synthesis at rest as well as a magnified effect after exercise.
HMB Benefits for Muscle Strength, Recovery, and Healthy Aging
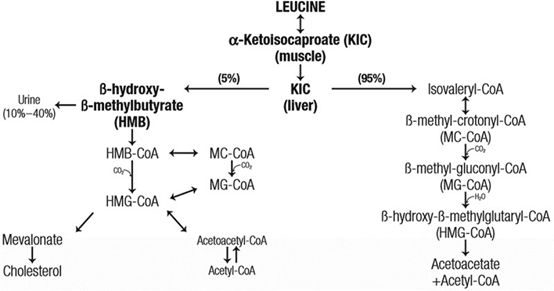
Another molecule that is worth tucking into your intervention arsenal is HMB. It’s an active metabolite of leucine. We convert about 5% of dietary leucine to HMB (see the graphic below). Taking HMB (as calcium-HMB) instead of leucine gives us more of this helpful metabolite without having to add a larger leucine/protein supplement (although since they appear to work via different mechanisms, combining leucine and HMB wouldn’t be redundant).
HMB is primarily used in sports nutrition to reduce post exercise muscle damage/inflammation, increase lean body mass, and improve strength and aerobic capacity. Typically dosing is 3 g/d for 3-4 weeks. Some research has used up to 6 g, although this doesn’t seem to confer any additional benefit (and also no observable risks). The International Society of Sports Nutrition has published their own position statement on HMB*, recommending dosing at 38 mg/kg body weight in combination with exercise training to increase lean body mass.
Beyond sports nutrition, the same International Society of Sports Nutrition states that HMB “may be important in a non-exercising sedentary and aging population to improve muscle strength, functionality, and muscle quality,” and that HMB may help “counter muscle atrophy during periods of inactivity due to illness or injury.”
In a controlled study in older adults, HMB for 12 weeks improved handgrip strength, gait speed, standing test and muscle quality even without changing muscle mass*. In a double-blind study of middle-aged women, 12 weeks of HMB plus vitamin D decreased intermuscular adipose tissue*, independent of exercise status. If you’ve listened to my recent conversation with Dr. Lyon, you’ll know the potential harm from this to-date underaddressed issue in derailing metabolic health.
Vitamin D and Muscle Function: What the Research Shows
Don’t miss that vitamin D addition in the study above, too. Of course, declines in vitamin D status and muscle function often go hand in hand with age, but vitamin D deficiency has been specifically linked with worse upper and lower limb muscle strength in postmenopausal women. Skeletal muscle cells have vitamin D receptors and polymorphisms in genes related to vitamin D transport and metabolism have been associated with different muscle phenotypes.
So far, however, intervention studies using vitamin D haven’t shown a consistent benefit either for post-exercise muscle recovery or muscle strength in older individuals. Baseline status, surprisingly rarely considered in clinical trials, may make a difference. As may dosing and the duration of exposure necessary to impact muscle performance.
One interesting vitamin D-related consideration is its potential ability to inhibit fat infiltration into muscle cells. This has only been seen so far in preclinical/in-vitro models, but given the impact of intramuscular adiposity on metabolic health and muscle strength, I think this is a noteworthy connection.
The bottom line is we can’t omit our foundational workhorse nutrients like vitamin D.
The Gut-Muscle Axis: How the Microbiome Influences Muscle Health and Aging
In general, and like many aspects of healthy aging, the gut microbiota and age-related sarcopenia are closely linked. The microbial production of short-chain fatty acids, urolithin A, and secondary bile acids are considered potentially pivotal factors in the gut-muscle axis.
There’s interesting data on urolithin A in particular. Urolithin A is a postbiotic compound derived from ellagic acid (ellagic acid is found in pomegranate, nuts, and seeds) via the microbiome. Its production is heavily influenced by the gut microbiota composition and while certain species such as Bifidobacterium pseudocatenulatum INIA P815 and Enterococcus faecium FUA027 have been shown to be likely urolithin A producers, research into the network of species (and there are likely multiple) involved in this multi-step process is still ongoing.
The bottom line, however, is that only around 40 percent of us appear to have a microbiome that produces urolithin A, making it something that I do consider supplementally. Clinical research has so far indicated that supplemental administration can improve mitophagy and muscle function, as well as lower CRP and inflammation.
Let us know your thoughts and questions below.
Additional DrKF Resources
- Blog: The Protein Magic Formula: How Much Should We Eat For Optimal Health & Longevity?
- Blog: Creatine Benefits Beyond Muscle: Emerging Research on Brain Health, Metabolism, and Longevity
- Blog: Is Creatine Safe? What Clinicians Need to Know About Side Effects, Dosing, and Longevity Benefits
- Blog: Human Clinical Evidence Supporting High-Dose Urolithin A for Mitochondrial and Immune Function
- Webinar: Strategies to Restore Mitochondrial Function and Support Healthy Aging: The Role of Urolithin A
- Podcast: Why Aging Is Not a Fat Problem — A Muscle-Centric Approach to Longevity
- Podcast: The Bile Acid Imbalance Accelerating Aging: How to Detect & Fix It
- Podcast: When High Protein Backfires in the Gut | Dr. Tom Fabian
